46 results
Data-driven healthcare indicators via precision gaming: With application to India
- Chih-Hao Huang, Namita Mohandas, Aparna Raj, Susan Howard, Feras A. Batarseh
-
- Journal:
- Data & Policy / Volume 6 / 2024
- Published online by Cambridge University Press:
- 01 April 2024, e22
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Precision healthcare is an emerging field of science that utilizes an individual’s health information, context, and genetics to provide more personalized diagnostics and treatments. In this manuscript, we leverage that concept and present a group of machine learning models for precision gaming. These predictive models guide adolescents through best practices related to their health. The use case deployed is for girls in India through a mobile application released in three different Indian states. To evaluate the usability of the models, experiments are designed and data (demographic, behavioral, and health-related) are collected. The experimental results are presented and discussed.
Implementation of contact precautions for multidrug-resistant organisms in the post–COVID-19 pandemic era: An updated national Emerging Infections Network (EIN) survey
- Jessica R. Howard-Anderson, Lindsey B. Gottlieb, Susan E. Beekmann, Philip M. Polgreen, Jesse T. Jacob, Daniel Z. Uslan
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 14 February 2024, pp. 1-6
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To understand how healthcare facilities employ contact precautions for patients with multidrug-resistant organisms (MDROs) in the post–coronavirus disease 2019 (COVID-19) era and explore changes since 2014.
Design:Cross-sectional survey.
Participants:Emerging Infections Network (EIN) physicians involved in infection prevention or hospital epidemiology.
Methods:In September 2022, we sent via email an 8-question survey on contact precautions and adjunctive measures to reduce MDRO transmission in inpatient facilities. We also asked about changes since the COVID-19 pandemic. We used descriptive statistics to summarize data and compared results to a similar survey administered in 2014.
Results:Of 708 EIN members, 283 (40%) responded to the survey and 201 reported working in infection prevention. A majority of facilities (66% and 69%) routinely use contact precautions for methicillin-resistant Staphylococcus aureus (MRSA) and vancomycin-resistant enterococci (VRE) respectively, compared to 93% and 92% in 2014. Nearly all (>90%) use contact precautions for Candida auris, carbapenem-resistant Enterobacterales (CRE), and carbapenem-resistant Acinetobacter baumannii. More variability was reported for carbapenem-resistant Pseudomonas aeruginosa and extended-spectrum β-lactamase–producing gram-negative organisms. Compared to 2014, fewer hospitals perform active surveillance for MRSA and VRE. Overall, 90% of facilities used chlorhexidine gluconate bathing in all or select inpatients, and 53% used ultraviolet light or hydrogen peroxide vapor disinfection at discharge. Many respondents (44%) reported changes to contact precautions since COVID-19 that remain in place.
Conclusions:Heterogeneity exists in the use of transmission-based precautions and adjunctive infection prevention measures aimed at reducing MDRO transmission. This variation reflects a need for updated and specific guidance, as well as further research on the use of contact precautions in healthcare facilities.
Assessment of perinatal anxiety: diagnostic accuracy of five measures
- Susan Ayers, Rose Coates, Andrea Sinesi, Helen Cheyne, Margaret Maxwell, Catherine Best, Stacey McNicol, Louise R. Williams, Nazihah Uddin, Una Hutton, Grace Howard, Judy Shakespeare, James J. Walker, Fiona Alderdice, Julie Jomeen, the MAP Study Team
-
- Journal:
- The British Journal of Psychiatry / Volume 224 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 132-138
- Print publication:
- April 2024
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Anxiety in pregnancy and after giving birth (the perinatal period) is highly prevalent but under-recognised. Robust methods of assessing perinatal anxiety are essential for services to identify and treat women appropriately.
AimsTo determine which assessment measures are most psychometrically robust and effective at identifying women with perinatal anxiety (primary objective) and depression (secondary objective).
MethodWe conducted a prospective longitudinal cohort study of 2243 women who completed five measures of anxiety and depression (Generalized Anxiety Disorder scale (GAD) two- and seven-item versions; Whooley questions; Clinical Outcomes in Routine Evaluation (CORE-10); and Stirling Antenatal Anxiety Scale (SAAS)) during pregnancy (15 weeks, 22 weeks and 31 weeks) and after birth (6 weeks). To assess diagnostic accuracy a sample of 403 participants completed modules of the Mini-International Neuropsychiatric Interview (MINI).
ResultsThe best diagnostic accuracy for anxiety was shown by the CORE-10 and SAAS. The best diagnostic accuracy for depression was shown by the CORE-10, SAAS and Whooley questions, although the SAAS had lower specificity. The same cut-off scores for each measure were optimal for identifying anxiety or depression (SAAS ≥9; CORE-10 ≥9; Whooley ≥1). All measures were psychometrically robust, with good internal consistency, convergent validity and unidimensional factor structure.
ConclusionsThis study identified robust and effective methods of assessing perinatal anxiety and depression. We recommend using the CORE-10 or SAAS to assess perinatal anxiety and the CORE-10 or Whooley questions to assess depression. The GAD-2 and GAD-7 did not perform as well as other measures and optimal cut-offs were lower than currently recommended.
Community engagement and financial arrangements: Navigating institutional change
- Linda Sprague Martinez, Riana C. Howard, Marieka Schotland, Rebecca Lobb, Tracy Battaglia, Susan Stone, Coco Auerswald, Emily Ozer
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 16 November 2023, e261
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Despite their documented benefits, the widespread adoption of community-engaged and participatory approaches among health researchers remains limited. Institutional practices and policies influence the uptake of community engagement and participatory approaches. We examine the role of financial arrangements between university researchers and community partners, by exploring efforts to bridge the gap between research administration and researchers at two research-intensive institutions. The type of financial arrangement a researcher has with a community partner plays an important role in setting the stage for the structure of the partnership as it relates to shared decision-making and ownership of the research. Continued efforts to clarify and streamline subcontracting processes are needed as is infrastructure to support community partners and researchers as they navigate financial arrangements if progress is to be made.
Use of contact precautions for multidrug-resistant organisms and the impact of the COVID-19 pandemic: An Emerging Infections Network (EIN) survey
- Jessica Howard-Anderson, Lindsey Gottlieb, Susan E. Beekmann, Philip Polgreen, Jesse T. Jacob, Daniel Z. Uslan
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s102-s103
-
- Article
-
- You have access Access
- Open access
- Export citation
-
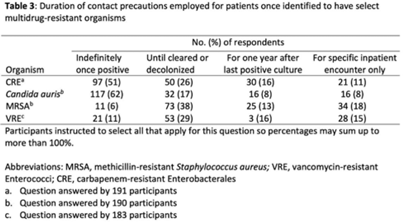
Background: The CDC recommends routine use of contact precautions for patients infected or colonized with multidrug-resistant organisms (MDROs). There is variability in implementation of and adherence to this recommendation, which we hypothesized may have been exacerbated by the COVID-19 pandemic. Methods: In September 2022, we emailed an 8-question survey to Emerging Infections Network (EIN) physician members with infection prevention and hospital epidemiology responsibilities. The survey asked about the respondent’s primary hospital’s recommendations on transmission-based precautions, adjunctive measures to reduce MDRO transmission, and changes that occurred during the COVID-19 pandemic. We sent 2 reminder emails over a 1-month period. We used descriptive statistics to summarize the data and to compare results to a similar EIN survey (n = 336) administered in 2014 (Russell D, et al. doi:10.1017/ice.2015.246). Results: Of 708 EIN members, 283 (40%) responded to the survey, and 201 were involved in infection prevention. Most respondents were adult infectious diseases physicians (n = 228, 80%) with at least 15 years of experience (n = 174, 63%). Respondents were well distributed among community, academic, and nonuniversity teaching facilities (Table 1). Most respondents reported that their facility routinely used CP for methicillin-resistant Staphylococcus aureus (MRSA, 66%) and vancomycin-resistant Enterococcus (VRE, 69%), compared to 93% and 92% respectively, in the 2014 survey. Nearly all (>90%) reported using contact precautions for Candida auris, carbapenem-resistant Enterobacterales (CRE), and carbapenem-resistant Acinetobacter spp, but there was variability in the use of contact precautions for carbapenem-resistant Pseudomonas aeruginosa and extended-spectrum β-lactamase–producing gram-negative organisms. In 2014, 81% reported that their hospital performed active surveillance testing for MRSA, and in 2022 this rate fell to 54% (Table 2). The duration of contact precautions varied by MDRO (Table 3). Compared to 2014, in 2022 facilities were less likely to use contact precautions indefinitely for MRSA (18% vs 6%) and VRE (31% vs 11%). Also, 180 facilities (90%) performed chlorhexidine bathing in at least some inpatients and 106 facilities (53%) used ultraviolet light or hydrogen peroxide vapor disinfection at discharge in some rooms. Furthermore, 89 facilities (44%) reported institutional changes to contact precautions policies after the start of the COVID-19 pandemic that remain in place. Conclusions: Use of contact precautions for patients with MDROs is heterogenous, and policies vary based on the organism. Although most hospitals still routinely use contact precautions for MRSA and VRE, this practice has declined substantially since 2014. Changes in contact-precaution policies may have been influenced by the COVID-19 pandemic, and more specifically, contemporary public health guidance is needed to define who requires contact precautions and for what duration.
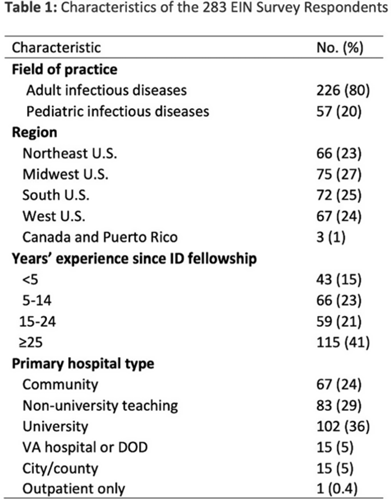
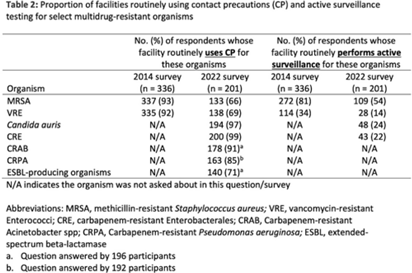

Disclosures: None
Mother–infant interaction and infant development in women at risk of postpartum psychosis with and without a postpartum relapse
- Alessandra Biaggi, Katie Hazelgrove, Freddie Waites, Rebecca H. Bind, Andrew J. Lawrence, Montserrat Fuste, Susan Conroy, Louise M. Howard, Mitul A. Mehta, Maddalena Miele, Gertrude Seneviratne, Susan Pawlby, Carmine M. Pariante, Paola Dazzan
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 4 / March 2024
- Published online by Cambridge University Press:
- 14 September 2023, pp. 823-834
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
This study aimed to investigate mother–infant interaction and infant development in women at-risk of postpartum psychosis (PP), with and without a postpartum relapse.
Methods103 women (and their offspring) were included, 43 at-risk-of-PP because of a diagnosis of bipolar disorder, schizoaffective disorder or previous PP, and 60 with no current/previous mental illness or family history of PP. Of the at-risk women, 18 developed a psychiatric relapse within 4 weeks after delivery (AR-unwell), while 25 remained symptom-free (AR-well). Mother–infant interaction was assessed using the CARE-Index at 8 weeks' and 12 months' postpartum and infant development using the Bayley-III at 12 months' postpartum.
ResultsWomen at-risk-of-PP as a group, regardless of whether they developed a psychiatric relapse within 4 weeks after delivery, had less synchronous mother–infant interactions and had infants with less optimal cognitive, language, motor and socio-emotional development than healthy controls. In particular, boys of at-risk women had the lowest scores in cognitive, language and motor development and in mother–infant interaction, while girls of the at-risk women had the lowest scores in socio-emotional development. The synchrony in the dyad predicted infant cognitive and language development. There was no evidence for a difference in mother–infant interaction nor in infant development between the AR-unwell and AR-well groups.
ConclusionsThese results suggest that, while there is a lack of evidence that an early postpartum relapse in women at-risk-of-PP could represent a risk for the infant per se, maternal risk for PP may be associated with less optimal mother–infant interaction and infant development.
Effectiveness and cost-effectiveness of psychiatric mother and baby units: quasi-experimental study – CORRIGENDUM
- Louise M. Howard, Kylee Trevillion, Laura Potts, Margaret Heslin, Andrew Pickles, Sarah Byford, Lauren E. Carson, Clare Dolman, Stacey Jennings, Sonia Johnson, Ian Jones, Rebecca McDonald, Susan Pawlby, Claire Powell, Gertrude Seneviratne, Rebekah Shallcross, Nicky Stanley, Angelika Wieck, Kathryn M. Abel
-
- Journal:
- The British Journal of Psychiatry / Volume 221 / Issue 5 / November 2022
- Published online by Cambridge University Press:
- 03 August 2022, p. 704
- Print publication:
- November 2022
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Cost-effectiveness of mirtazapine for agitated behaviors in dementia: findings from a randomized controlled trial
- Catherine Henderson, Martin Knapp, Susan Stirling, Lee Shepstone, Juliet High, Clive Ballard, Peter Bentham, Alistair Burns, Nicolas Farina, Chris Fox, Julia Fountain, Paul Francis, Robert Howard, Iracema Leroi, Gill Livingston, Ramin Nilforooshan, Shirley Nurock, John T. O’Brien, Annabel Price, Ann Marie Swart, Naji Tabet, Tanya Telling, Alan J. Thomas, Sube Banerjee
-
- Journal:
- International Psychogeriatrics / Volume 34 / Issue 10 / October 2022
- Published online by Cambridge University Press:
- 19 July 2022, pp. 905-917
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objectives:
To examine the costs and cost-effectiveness of mirtazapine compared to placebo over 12-week follow-up.
Design:Economic evaluation in a double-blind randomized controlled trial of mirtazapine vs. placebo.
Setting:Community settings and care homes in 26 UK centers.
Participants:People with probable or possible Alzheimer’s disease and agitation.
Measurements:Primary outcome included incremental cost of participants’ health and social care per 6-point difference in CMAI score at 12 weeks. Secondary cost-utility analyses examined participants’ and unpaid carers’ gain in quality-adjusted life years (derived from EQ-5D-5L, DEMQOL-Proxy-U, and DEMQOL-U) from the health and social care and societal perspectives.
Results:One hundred and two participants were allocated to each group; 81 mirtazapine and 90 placebo participants completed a 12-week assessment (87 and 95, respectively, completed a 6-week assessment). Mirtazapine and placebo groups did not differ on mean CMAI scores or health and social care costs over the study period, before or after adjustment for center and living arrangement (independent living/care home). On the primary outcome, neither mirtazapine nor placebo could be considered a cost-effective strategy with a high level of confidence. Groups did not differ in terms of participant self- or proxy-rated or carer self-rated quality of life scores, health and social care or societal costs, before or after adjustment.
Conclusions:On cost-effectiveness grounds, the use of mirtazapine cannot be recommended for agitated behaviors in people living with dementia. Effective and cost-effective medications for agitation in dementia remain to be identified in cases where non-pharmacological strategies for managing agitation have been unsuccessful.
Effectiveness and cost-effectiveness of psychiatric mother and baby units: quasi-experimental study
- Louise M. Howard, Kylee Trevillion, Laura Potts, Margaret Heslin, Andrew Pickles, Sarah Byford, Lauren E. Carson, Clare Dolman, Stacey Jennings, Sonia Johnson, Ian Jones, Rebecca McDonald, Susan Pawlby, Claire Powell, Gertrude Seneviratne, Rebekah Shallcross, Nicky Stanley, Angelika Wieck, Kathryn M. Abel
-
- Journal:
- The British Journal of Psychiatry / Volume 221 / Issue 4 / October 2022
- Published online by Cambridge University Press:
- 04 May 2022, pp. 628-636
- Print publication:
- October 2022
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Psychiatric mother and baby units (MBUs) are recommended for severe perinatal mental illness, but effectiveness compared with other forms of acute care remains unknown.
AimsWe hypothesised that women admitted to MBUs would be less likely to be readmitted to acute care in the 12 months following discharge, compared with women admitted to non-MBU acute care (generic psychiatric wards or crisis resolution teams (CRTs)).
MethodQuasi-experimental cohort study of women accessing acute psychiatric care up to 1 year postpartum in 42 healthcare organisations across England and Wales. Primary outcome was readmission within 12 months post-discharge. Propensity scores were used to account for systematic differences between MBU and non-MBU participants. Secondary outcomes included assessment of cost-effectiveness, experience of services, unmet needs, perceived bonding, observed mother–infant interaction quality and safeguarding outcome.
ResultsOf 279 women, 108 (39%) received MBU care, 62 (22%) generic ward care and 109 (39%) CRT care only. The MBU group (n = 105) had similar readmission rates to the non-MBU group (n = 158) (aOR = 0.95, 95% CI 0.86–1.04, P = 0.29; an absolute difference of −5%, 95% CI −14 to 4%). Service satisfaction was significantly higher among women accessing MBUs compared with non-MBUs; no significant differences were observed for any other secondary outcomes.
ConclusionsWe found no significant differences in rates of readmission, but MBU advantage might have been masked by residual confounders; readmission will also depend on quality of care after discharge and type of illness. Future studies should attempt to identify the effective ingredients of specialist perinatal in-patient and community care to improve outcomes.
Characterisation of age and polarity at onset in bipolar disorder
- Janos L. Kalman, Loes M. Olde Loohuis, Annabel Vreeker, Andrew McQuillin, Eli A. Stahl, Douglas Ruderfer, Maria Grigoroiu-Serbanescu, Georgia Panagiotaropoulou, Stephan Ripke, Tim B. Bigdeli, Frederike Stein, Tina Meller, Susanne Meinert, Helena Pelin, Fabian Streit, Sergi Papiol, Mark J. Adams, Rolf Adolfsson, Kristina Adorjan, Ingrid Agartz, Sofie R. Aminoff, Heike Anderson-Schmidt, Ole A. Andreassen, Raffaella Ardau, Jean-Michel Aubry, Ceylan Balaban, Nicholas Bass, Bernhard T. Baune, Frank Bellivier, Antoni Benabarre, Susanne Bengesser, Wade H Berrettini, Marco P. Boks, Evelyn J. Bromet, Katharina Brosch, Monika Budde, William Byerley, Pablo Cervantes, Catina Chillotti, Sven Cichon, Scott R. Clark, Ashley L. Comes, Aiden Corvin, William Coryell, Nick Craddock, David W. Craig, Paul E. Croarkin, Cristiana Cruceanu, Piotr M. Czerski, Nina Dalkner, Udo Dannlowski, Franziska Degenhardt, Maria Del Zompo, J. Raymond DePaulo, Srdjan Djurovic, Howard J. Edenberg, Mariam Al Eissa, Torbjørn Elvsåshagen, Bruno Etain, Ayman H. Fanous, Frederike Fellendorf, Alessia Fiorentino, Andreas J. Forstner, Mark A. Frye, Janice M. Fullerton, Katrin Gade, Julie Garnham, Elliot Gershon, Michael Gill, Fernando S. Goes, Katherine Gordon-Smith, Paul Grof, Jose Guzman-Parra, Tim Hahn, Roland Hasler, Maria Heilbronner, Urs Heilbronner, Stephane Jamain, Esther Jimenez, Ian Jones, Lisa Jones, Lina Jonsson, Rene S. Kahn, John R. Kelsoe, James L. Kennedy, Tilo Kircher, George Kirov, Sarah Kittel-Schneider, Farah Klöhn-Saghatolislam, James A. Knowles, Thorsten M. Kranz, Trine Vik Lagerberg, Mikael Landen, William B. Lawson, Marion Leboyer, Qingqin S. Li, Mario Maj, Dolores Malaspina, Mirko Manchia, Fermin Mayoral, Susan L. McElroy, Melvin G. McInnis, Andrew M. McIntosh, Helena Medeiros, Ingrid Melle, Vihra Milanova, Philip B. Mitchell, Palmiero Monteleone, Alessio Maria Monteleone, Markus M. Nöthen, Tomas Novak, John I. Nurnberger, Niamh O'Brien, Kevin S. O'Connell, Claire O'Donovan, Michael C. O'Donovan, Nils Opel, Abigail Ortiz, Michael J. Owen, Erik Pålsson, Carlos Pato, Michele T. Pato, Joanna Pawlak, Julia-Katharina Pfarr, Claudia Pisanu, James B. Potash, Mark H Rapaport, Daniela Reich-Erkelenz, Andreas Reif, Eva Reininghaus, Jonathan Repple, Hélène Richard-Lepouriel, Marcella Rietschel, Kai Ringwald, Gloria Roberts, Guy Rouleau, Sabrina Schaupp, William A Scheftner, Simon Schmitt, Peter R. Schofield, K. Oliver Schubert, Eva C. Schulte, Barbara Schweizer, Fanny Senner, Giovanni Severino, Sally Sharp, Claire Slaney, Olav B. Smeland, Janet L. Sobell, Alessio Squassina, Pavla Stopkova, John Strauss, Alfonso Tortorella, Gustavo Turecki, Joanna Twarowska-Hauser, Marin Veldic, Eduard Vieta, John B. Vincent, Wei Xu, Clement C. Zai, Peter P. Zandi, Psychiatric Genomics Consortium (PGC) Bipolar Disorder Working Group, International Consortium on Lithium Genetics (ConLiGen), Colombia-US Cross Disorder Collaboration in Psychiatric Genetics, Arianna Di Florio, Jordan W. Smoller, Joanna M. Biernacka, Francis J. McMahon, Martin Alda, Bertram Müller-Myhsok, Nikolaos Koutsouleris, Peter Falkai, Nelson B. Freimer, Till F.M. Andlauer, Thomas G. Schulze, Roel A. Ophoff
-
- Journal:
- The British Journal of Psychiatry / Volume 219 / Issue 6 / December 2021
- Published online by Cambridge University Press:
- 25 August 2021, pp. 659-669
- Print publication:
- December 2021
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Studying phenotypic and genetic characteristics of age at onset (AAO) and polarity at onset (PAO) in bipolar disorder can provide new insights into disease pathology and facilitate the development of screening tools.
AimsTo examine the genetic architecture of AAO and PAO and their association with bipolar disorder disease characteristics.
MethodGenome-wide association studies (GWASs) and polygenic score (PGS) analyses of AAO (n = 12 977) and PAO (n = 6773) were conducted in patients with bipolar disorder from 34 cohorts and a replication sample (n = 2237). The association of onset with disease characteristics was investigated in two of these cohorts.
ResultsEarlier AAO was associated with a higher probability of psychotic symptoms, suicidality, lower educational attainment, not living together and fewer episodes. Depressive onset correlated with suicidality and manic onset correlated with delusions and manic episodes. Systematic differences in AAO between cohorts and continents of origin were observed. This was also reflected in single-nucleotide variant-based heritability estimates, with higher heritabilities for stricter onset definitions. Increased PGS for autism spectrum disorder (β = −0.34 years, s.e. = 0.08), major depression (β = −0.34 years, s.e. = 0.08), schizophrenia (β = −0.39 years, s.e. = 0.08), and educational attainment (β = −0.31 years, s.e. = 0.08) were associated with an earlier AAO. The AAO GWAS identified one significant locus, but this finding did not replicate. Neither GWAS nor PGS analyses yielded significant associations with PAO.
ConclusionsAAO and PAO are associated with indicators of bipolar disorder severity. Individuals with an earlier onset show an increased polygenic liability for a broad spectrum of psychiatric traits. Systematic differences in AAO across cohorts, continents and phenotype definitions introduce significant heterogeneity, affecting analyses.
Association of Ventilation during Initial Trauma Resuscitation for Traumatic Brain Injury and Post-Traumatic Outcomes: A Systematic Review
- Mary Beth Howard, Nichole McCollum, Emily C. Alberto, Hannah Kotler, Mary E. Mottla, Laura Tiusaba, Susan Keller, Ivan Marsic, Aleksandra Sarcevic, Randall S. Burd, Karen J. O’Connell
-
- Journal:
- Prehospital and Disaster Medicine / Volume 36 / Issue 4 / August 2021
- Published online by Cambridge University Press:
- 31 May 2021, pp. 460-465
- Print publication:
- August 2021
-
- Article
- Export citation
-
Objectives:
In the absence of evidence of acute cerebral herniation, normal ventilation is recommended for patients with traumatic brain injury (TBI). Despite this recommendation, ventilation strategies vary during the initial management of patients with TBI and may impact outcome. The goal of this systematic review was to define the best evidence-based practice of ventilation management during the initial resuscitation period.
Methods:A literature search of PubMed, CINAHL, and SCOPUS identified studies from 2009 through 2019 addressing the effects of ventilation during the initial post-trauma resuscitation on patient outcomes.
Results:The initial search yielded 899 articles, from which 13 were relevant and selected for full-text review. Six of the 13 articles met the inclusion criteria, all of which reported on patients with TBI. Either end-tidal carbon dioxide (ETCO2) or partial pressure carbon dioxide (PCO2) were the independent variables associated with mortality. Decreased rates of mortality were reported in patients with normal PCO2 or ETCO2.
Conclusions:Normoventilation, as measured by ETCO2 or PCO2, is associated with decreased mortality in patients with TBI. Preventing hyperventilation or hypoventilation in patients with TBI during the early resuscitation phase could improve outcome after TBI.
A new tide model for the Antarctic ice shelves and seas
- Laurie Padman, Helen A. Fricker, Richard Coleman, Susan Howard, Lana Erofeeva
-
- Journal:
- Annals of Glaciology / Volume 34 / 2002
- Published online by Cambridge University Press:
- 14 September 2017, pp. 247-254
-
- Article
-
- You have access Access
- HTML
- Export citation
-
We describe a new tide model for the seas surrounding Antarctica, including the ocean cavities under the floating ice shelves. The model uses data assimilation to improve its fit to available data. Typical peak-to-peak tide ranges on ice shelves are 1–2 m but can exceed 3 m for the Filchner–Ronne and Larsen Ice Shelves in the Weddell Sea. Spring tidal ranges are about twice these values. Model performance is judged relative to the ~5–10 cm accuracy that is needed to fully utilize ice-shelf height data that will be collected with the Geoscience Laser Altimeter System, scheduled to be launched on the Ice, Cloud and land Elevation Satellite in late 2002. The model does not yet achieve this level of accuracy except very near the few high-quality tidal records that have been assimilated into the model. Some improvement in predictive skill is expected from increased sophistication of model physics, but we also require better definition of ice-shelf grounding lines and more accurate water-column thickness data in shelf seas and under the ice shelves. Long-duration tide measurements (bottom pressure gauge or global positioning system) in critical data-sparse areas, particularly near and on the Filchner–Ronne and Ross Ice Shelves and Pine Island Bay, are required to improve the performance of the data-assimilation model.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Contributors
-
- By Rony A. Adam, Gloria Bachmann, Nichole M. Barker, Randall B. Barnes, John Bennett, Inbar Ben-Shachar, Jonathan S. Berek, Sarah L. Berga, Monica W. Best, Eric J. Bieber, Frank M. Biro, Shan Biscette, Anita K. Blanchard, Candace Brown, Ronald T. Burkman, Joseph Buscema, John E. Buster, Michael Byas-Smith, Sandra Ann Carson, Judy C. Chang, Annie N. Y. Cheung, Mindy S. Christianson, Karishma Circelli, Daniel L. Clarke-Pearson, Larry J. Copeland, Bryan D. Cowan, Navneet Dhillon, Michael P. Diamond, Conception Diaz-Arrastia, Nicole M. Donnellan, Michael L. Eisenberg, Eric Eisenhauer, Sebastian Faro, J. Stuart Ferriss, Lisa C. Flowers, Susan J. Freeman, Leda Gattoc, Claudine Marie Gayle, Timothy M. Geiger, Jennifer S. Gell, Alan N. Gordon, Victoria L. Green, Jon K. Hathaway, Enrique Hernandez, S. Paige Hertweck, Randall S. Hines, Ira R. Horowitz, Fred M. Howard, William W. Hurd, Fidan Israfilbayli, Denise J. Jamieson, Carolyn R. Jaslow, Erika B. Johnston-MacAnanny, Rohna M. Kearney, Namita Khanna, Caroline C. King, Jeremy A. King, Ira J. Kodner, Tamara Kolev, Athena P. Kourtis, S. Robert Kovac, Ertug Kovanci, William H. Kutteh, Eduardo Lara-Torre, Pallavi Latthe, Herschel W. Lawson, Ronald L. Levine, Frank W. Ling, Larry I. Lipshultz, Steven D. McCarus, Robert McLellan, Shruti Malik, Suketu M. Mansuria, Mohamed K. Mehasseb, Pamela J. Murray, Saloney Nazeer, Farr R. Nezhat, Hextan Y. S. Ngan, Gina M. Northington, Peggy A. Norton, Ruth M. O'Regan, Kristiina Parviainen, Resad P. Pasic, Tanja Pejovic, K. Ulrich Petry, Nancy A. Phillips, Ashish Pradhan, Elizabeth E. Puscheck, Suneetha Rachaneni, Devon M. Ramaeker, David B. Redwine, Robert L. Reid, Carla P. Roberts, Walter Romano, Peter G. Rose, Robert L. Rosenfield, Shon P. Rowan, Mack T. Ruffin, Janice M. Rymer, Evis Sala, Ritu Salani, Joseph S. Sanfilippo, Mahmood I. Shafi, Roger P. Smith, Meredith L. Snook, Thomas E. Snyder, Mary D. Stephenson, Thomas G. Stovall, Richard L. Sweet, Philip M. Toozs-Hobson, Togas Tulandi, Elizabeth R. Unger, Denise S. Uyar, Marion S. Verp, Rahi Victory, Tamara J. Vokes, Michelle J. Washington, Katharine O'Connell White, Paul E. Wise, Frank M. Wittmaack, Miya P. Yamamoto, Christine Yu, Howard A. Zacur
- Edited by Eric J. Bieber, Joseph S. Sanfilippo, University of Pittsburgh, Ira R. Horowitz, Emory University, Atlanta, Mahmood I. Shafi
-
- Book:
- Clinical Gynecology
- Published online:
- 05 April 2015
- Print publication:
- 23 April 2015, pp viii-xiv
-
- Chapter
- Export citation
Recommendations of the Canadian Consensus Conference on Dementia - Dissemination, Implementation, and Evaluation of Impact
- David B. Hogan, Penny Jennett, Susan Freter, Howard Bergman, Howard Chertkow, Susan Gold, A. Mark Clarfield
-
- Journal:
- Canadian Journal of Neurological Sciences / Volume 28 / Issue S1 / May 2001
- Published online by Cambridge University Press:
- 02 December 2014, pp. S115-S121
-
- Article
-
- You have access Access
- Export citation
-
Background:
Subsequent to the development of consensus statements on a clinical topic, it is vital to establish a plan for dissemination, implementation and evaluation of impact. Consensus statements can be used for both guiding continuing medical education (CME) and producing clinical practice guidelines (CPGs). Insufficient attention to dissemination can lead to a failure to change physician behaviour and improve patient outcomes.
Methods:A plan to disseminate the conclusions of the Canadian Consensus Conference on Dementia (CCCD) was developed. This plan was based on a literature review of CME and CPGs. A Medline search was performed on the dissemination and evaluation of the 1989 Canadian Consensus Conference on the Assessment of Dementia (CCCAD) and other published guides for physicians on dementia care. CCCD dissemination that has occurred to date (June, 2000) was reviewed in this paper.
Results:Lectures and unsolicited printed material are weak forms of CME. Small-group interactive CME that provides practice opportunities appears to be the most effective way to change physician behaviour. The ability of CPGs to change physician behaviour is uncertain. It appears that inadequate attention has been placed on CPG dissemination and implementation. The CCCAD had a modest impact on clinical practice in Canada. While dissemination of the conclusions of the CCCD has taken place, evaluation of the impact of the CCCD has yet to be done. Local initiatives utilizing the conclusions of the CCCD are on-going.
Conclusion:Further work is needed on how to optimize the impact of consensus statements and CPGs. While dissemination of the CCCD has occurred, it is currently unknown whether it has led to any change in physician practices.
Contributors
-
- By Rim-Sarah Alouane, Schirin Amir-Moazami, Naima Bouteldja, Emmanuelle Bribosia, Eva Brems, Susan Edwards, Nadia Fadil, Erica Howard, Yaiza Janssens, Kim Lecoyer, Maleiha Malik, Annelies Moors, Saïla Ouald Chaib, Kate Østergaard, Isabelle Rorive, Birgitte Schepelern Johansen, Dolores Morondo Taramundi, Victoria Vandersteen, Jogchum Vrielink, Margit Warburg
- Edited by Eva Brems, Universiteit Gent, Belgium
-
- Book:
- The Experiences of Face Veil Wearers in Europe and the Law
- Published online:
- 05 September 2014
- Print publication:
- 11 September 2014, pp vii-viii
-
- Chapter
- Export citation
Contributors
-
- By Lenard A. Adler, Pinky Agarwal, Rehan Ahmed, Jagga Rao Alluri, Fawaz Al-Mufti, Samuel Alperin, Michael Amoashiy, Michael Andary, David J. Anschel, Padmaja Aradhya, Vandana Aspen, Esther Baldinger, Jee Bang, George D. Baquis, John J. Barry, Jason J. S. Barton, Julius Bazan, Amanda R. Bedford, Marlene Behrmann, Lourdes Bello-Espinosa, Ajay Berdia, Alan R. Berger, Mark Beyer, Don C. Bienfang, Kevin M. Biglan, Thomas M. Boes, Paul W. Brazis, Jonathan L. Brisman, Jeffrey A. Brown, Scott E. Brown, Ryan R. Byrne, Rina Caprarella, Casey A. Chamberlain, Wan-Tsu W. Chang, Grace M. Charles, Jasvinder Chawla, David Clark, Todd J. Cohen, Joe Colombo, Howard Crystal, Vladimir Dadashev, Sarita B. Dave, Jean Robert Desrouleaux, Richard L. Doty, Robert Duarte, Jeffrey S. Durmer, Christyn M. Edmundson, Eric R. Eggenberger, Steven Ender, Noam Epstein, Alberto J. Espay, Alan B. Ettinger, Niloofar (Nelly) Faghani, Amtul Farheen, Edward Firouztale, Rod Foroozan, Anne L. Foundas, David Elliot Friedman, Deborah I. Friedman, Steven J. Frucht, Oded Gerber, Tal Gilboa, Martin Gizzi, Teneille G. Gofton, Louis J. Goodrich, Malcolm H. Gottesman, Varda Gross-Tsur, Deepak Grover, David A. Gudis, John J. Halperin, Maxim D. Hammer, Andrew R. Harrison, L. Anne Hayman, Galen V. Henderson, Steven Herskovitz, Caitlin Hoffman, Laryssa A. Huryn, Andres M. Kanner, Gary P. Kaplan, Bashar Katirji, Kenneth R. Kaufman, Annie Killoran, Nina Kirz, Gad E. Klein, Danielle G. Koby, Christopher P. Kogut, W. Curt LaFrance, Patrick J.M. Lavin, Susan W. Law, James L. Levenson, Richard B. Lipton, Glenn Lopate, Daniel J. Luciano, Reema Maindiratta, Robert M. Mallery, Georgios Manousakis, Alan Mazurek, Luis J. Mejico, Dragana Micic, Ali Mokhtarzadeh, Walter J. Molofsky, Heather E. Moss, Mark L. Moster, Manpreet Multani, Siddhartha Nadkarni, George C. Newman, Rolla Nuoman, Paul A. Nyquist, Gaia Donata Oggioni, Odi Oguh, Denis Ostrovskiy, Kristina Y. Pao, Juwen Park, Anastas F. Pass, Victoria S. Pelak, Jeffrey Peterson, John Pile-Spellman, Misha L. Pless, Gregory M. Pontone, Aparna M. Prabhu, Michael T. Pulley, Philip Ragone, Prajwal Rajappa, Venkat Ramani, Sindhu Ramchandren, Ritesh A. Ramdhani, Ramses Ribot, Heidi D. Riney, Diana Rojas-Soto, Michael Ronthal, Daniel M. Rosenbaum, David B. Rosenfield, Durga Roy, Michael J. Ruckenstein, Max C. Rudansky, Eva Sahay, Friedhelm Sandbrink, Jade S. Schiffman, Angela Scicutella, Maroun T. Semaan, Robert C. Sergott, Aashit K. Shah, David M. Shaw, Amit M. Shelat, Claire A. Sheldon, Anant M. Shenoy, Yelizaveta Sher, Jessica A. Shields, Tanya Simuni, Rajpaul Singh, Eric E. Smouha, David Solomon, Mehri Songhorian, Steven A. Sparr, Egilius L. H. Spierings, Eve G. Spratt, Beth Stein, S.H. Subramony, Rosa Ana Tang, Cara Tannenbaum, Hakan Tekeli, Amanda J. Thompson, Michael J. Thorpy, Matthew J. Thurtell, Pedro J. Torrico, Ira M. Turner, Scott Uretsky, Ruth H. Walker, Deborah M. Weisbrot, Michael A. Williams, Jacques Winter, Randall J. Wright, Jay Elliot Yasen, Shicong Ye, G. Bryan Young, Huiying Yu, Ryan J. Zehnder
- Edited by Alan B. Ettinger, Albert Einstein College of Medicine, New York, Deborah M. Weisbrot, State University of New York, Stony Brook
-
- Book:
- Neurologic Differential Diagnosis
- Published online:
- 05 June 2014
- Print publication:
- 17 April 2014, pp xi-xx
-
- Chapter
- Export citation
Use of vitamin D supplements during infancy in an international feeding trial
- Eveliina Lehtonen, Anne Ormisson, Anita Nucci, David Cuthbertson, Susa Sorkio, Mila Hyytinen, Kirsi Alahuhta, Carol Berseth, Marja Salonen, Shayne Taback, Margaret Franciscus, Teba González-Frutos, Tuuli E Korhonen, Margaret L Lawson, Dorothy J Becker, Jeffrey P Krischer, Mikael Knip, Suvi M Virtanen, , Thomas Mandrup-Poulsen, Elias Arjas, Åke Lernmark, Barbara Schmidt, Jeffrey P. Krischer, Hans K. Åkerblom, Mila Hyytinen, Mikael Knip, Katriina Koski, Matti Koski, Eeva Pajakkala, Marja Salonen, David Cuthbertson, Jeffrey P. Krischer, Linda Shanker, Brenda Bradley, Hans-Michael Dosch, John Dupré, William Fraser, Margaret Lawson, Jeffrey L. Mahon, Mathew Sermer, Shayne P. Taback, Dorothy Becker, Margaret Franciscus, Anita Nucci, Jerry Palmer, Minna Pekkala, Suvi M. Virtanen, Jacki Catteau, Neville Howard, Patricia Crock, Maria Craig, Cheril L. Clarson, Lynda Bere, David Thompson, Daniel Metzger, Colleen Marshall, Jennifer Kwan, David K. Stephure, Daniele Pacaud, Wendy Schwarz, Rose Girgis, Marilyn Thompson, Shayne P. Taback, Daniel Catte, Margaret L. Lawson, Brenda Bradley, Denis Daneman, Mathew Sermer, Mary-Jean Martin, Valérie Morin, Lyne Frenette, Suzanne Ferland, Susan Sanderson, Kathy Heath, Céline Huot, Monique Gonthier, Maryse Thibeault, Laurent Legault, Diane Laforte, Elizabeth A. Cummings, Karen Scott, Tracey Bridger, Cheryl Crummell, Robyn Houlden, Adriana Breen, George Carson, Sheila Kelly, Koravangattu Sankaran, Marie Penner, Richard A. White, Nancy King, James Popkin, Laurie Robson, Eva Al Taji, Irena Aldhoon, Pavla Mendlova, Jan Vavrinec, Jan Vosahlo, Ludmila Brazdova, Jitrenka Venhacova, Petra Venhacova, Adam Cipra, Zdenka Tomsikova, Petra Krckova, Pavla Gogelova, Ülle Einberg, Mall-Anne Riikjärv, Anne Ormisson, Vallo Tillmann, Päivi Kleemola, Anna Parkkola, Heli Suomalainen, Anna-Liisa Järvenpää, Anu-Maaria Hämälainen, Hannu Haavisto, Sirpa Tenhola, Pentti Lautala, Pia Salonen, Susanna Aspholm, Heli Siljander, Carita Holm, Samuli Ylitalo, Raisa Lounamaa, Anja Nuuja, Timo Talvitie, Kaija Lindström, Hanna Huopio, Jouni Pesola, Riitta Veijola, Päivi Tapanainen, Abram Alar, Paavo Korpela, Marja-Liisa Käär, Taina Mustila, Ritva Virransalo, Päivi Nykänen, Bärbel Aschemeier, Thomas Danne, Olga Kordonouri, Dóra Krikovszky, László Madácsy, Yeganeh Manon Khazrai, Ernesto Maddaloni, Paolo Pozzilli, Carla Mannu, Marco Songini, Carine de Beaufort, Ulrike Schierloh, Jan Bruining, Margriet Bisschoff, Aleksander Basiak, Renata Wasikowa, Marta Ciechanowska, Grazyna Deja, Przemyslawa Jarosz-Chobot, Agnieszka Szadkowska, Katarzyna Cypryk, Malgorzata Zawodniak-Szalapska, Luis Castano, Teba Gonzalez Frutos, Mirentxu Oyarzabal, Manuel Serrano-Ríos, María Teresa Martínez-Larrad, Federico Gustavo Hawkins, Dolores Rodriguez Arnau, Johnny Ludvigsson, Malgorzata Smolinska Konefal, Ragnar Hanas, Bengt Lindblad, Nils-Osten Nilsson, Hans Fors, Maria Nordwall, Agne Lindh, Hans Edenwall, Jan Aman, Calle Johansson, Margrit Gadient, Eugen Schoenle, Dorothy Becker, Ashi Daftary, Margaret Franciscus, Carol Gilmour, Jerry Palmer, Rachel Taculad, Marilyn Tanner-Blasiar, Neil White, Uday Devaskar, Heather Horowitz, Lisa Rogers, Roxana Colon, Teresa Frazer, Jose Torres, Robin Goland, Ellen Greenberg, Maudene Nelson, Holly Schachner, Barney Softness, Jorma Ilonen, Massimo Trucco, Lynn Nichol, Erkki Savilahti, Taina Härkönen, Mikael Knip, Outi Vaarala, Kristiina Luopajärvi, Hans-Michael Dosch
-
- Journal:
- Public Health Nutrition / Volume 17 / Issue 4 / April 2014
- Published online by Cambridge University Press:
- 24 June 2013, pp. 810-822
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Objective
To examine the use of vitamin D supplements during infancy among the participants in an international infant feeding trial.
DesignLongitudinal study.
SettingInformation about vitamin D supplementation was collected through a validated FFQ at the age of 2 weeks and monthly between the ages of 1 month and 6 months.
SubjectsInfants (n 2159) with a biological family member affected by type 1 diabetes and with increased human leucocyte antigen-conferred susceptibility to type 1 diabetes from twelve European countries, the USA, Canada and Australia.
ResultsDaily use of vitamin D supplements was common during the first 6 months of life in Northern and Central Europe (>80 % of the infants), with somewhat lower rates observed in Southern Europe (>60 %). In Canada, vitamin D supplementation was more common among exclusively breast-fed than other infants (e.g. 71 % v. 44 % at 6 months of age). Less than 2 % of infants in the USA and Australia received any vitamin D supplementation. Higher gestational age, older maternal age and longer maternal education were study-wide associated with greater use of vitamin D supplements.
ConclusionsMost of the infants received vitamin D supplements during the first 6 months of life in the European countries, whereas in Canada only half and in the USA and Australia very few were given supplementation.
Contributors
-
- By Phillip L. Ackerman, Soon Ang, Susan M. Barnett, G. David Batty, Anna S. Beninger, Jillian Brass, Meghan M. Burke, Nancy Cantor, Priyanka B. Carr, David R. Caruso, Stephen J. Ceci, Lillia Cherkasskiy, Joanna Christodoulou, Andrew R. A. Conway, Christine E. Daley, Janet E. Davidson, Jim Davies, Katie Davis, Ian J. Deary, Colin G. DeYoung, Ron Dumont, Carol S. Dweck, Linn Van Dyne, Pascale M. J. Engel de Abreu, Joseph F. Fagan, David Henry Feldman, Kurt W. Fischer, Marisa H. Fisher, James R. Flynn, Liane Gabora, Howard Gardner, Glenn Geher, Sarah J. Getz, Judith Glück, Ashok K. Goel, Megan M. Griffin, Elena L. Grigorenko, Richard J. Haier, Diane F. Halpern, Christopher Hertzog, Robert M. Hodapp, Earl Hunt, Alan S. Kaufman, James C. Kaufman, Scott Barry Kaufman, Iris A. Kemp, John F. Kihlstrom, Joni M. Lakin, Christina S. Lee, David F. Lohman, N. J. Mackintosh, Brooke Macnamara, Samuel D. Mandelman, John D. Mayer, Richard E. Mayer, Martha J. Morelock, Ted Nettelbeck, Raymond S. Nickerson, Weihua Niu, Anthony J. Onwuegbuzie, Jonathan A. Plucker, Sally M. Reis, Joseph S. Renzulli, Heiner Rindermann, L. Todd Rose, Anne Russon, Peter Salovey, Scott Seider, Ellen L. Short, Keith E. Stanovich, Ursula M. Staudinger, Robert J. Sternberg, Carli A. Straight, Lisa A. Suzuki, Mei Ling Tan, Maggie E. Toplak, Susana Urbina, Richard K. Wagner, Richard F. West, Wendy M. Williams, John O. Willis, Thomas R. Zentall
- Edited by Robert J. Sternberg, Oklahoma State University, Scott Barry Kaufman, New York University
-
- Book:
- The Cambridge Handbook of Intelligence
- Published online:
- 05 June 2012
- Print publication:
- 30 May 2011, pp xi-xiv
-
- Chapter
- Export citation
Neuropsychological Profile of Parkin Mutation Carriers with and without Parkinson Disease: The CORE-PD Study
- Elise Caccappolo, Roy N. Alcalay, Helen Mejia-Santana, Ming-X. Tang, Brian Rakitin, Llency Rosado, Elan D. Louis, Cynthia L. Comella, Amy Colcher, Danna Jennings, Martha A. Nance, Susan Bressman, William K. Scott, Caroline M. Tanner, Susan F. Mickel, Howard F. Andrews, Cheryl Waters, Stanley Fahn, Lucien J. Cote, Steven Frucht, Blair Ford, Michael Rezak, Kevin Novak, Joseph H. Friedman, Ronald F. Pfeiffer, Laura Marsh, Brad Hiner, Andrew D. Siderowf, Barbara M. Ross, Miguel Verbitsky, Sergey Kisselev, Ruth Ottman, Lorraine N. Clark, Karen S. Marder
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 17 / Issue 1 / January 2011
- Published online by Cambridge University Press:
- 24 November 2010, pp. 91-100
-
- Article
- Export citation
-
The cognitive profile of early onset Parkinson’s disease (EOPD) has not been clearly defined. Mutations in the parkin gene are the most common genetic risk factor for EOPD and may offer information about the neuropsychological pattern of performance in both symptomatic and asymptomatic mutation carriers. EOPD probands and their first-degree relatives who did not have Parkinson’s disease (PD) were genotyped for mutations in the parkin gene and administered a comprehensive neuropsychological battery. Performance was compared between EOPD probands with (N = 43) and without (N = 52) parkin mutations. The same neuropsychological battery was administered to 217 first-degree relatives to assess neuropsychological function in individuals who carry parkin mutations but do not have PD. No significant differences in neuropsychological test performance were found between parkin carrier and noncarrier probands. Performance also did not differ between EOPD noncarriers and carrier subgroups (i.e., heterozygotes, compound heterozygotes/homozygotes). Similarly, no differences were found among unaffected family members across genotypes. Mean neuropsychological test performance was within normal range in all probands and relatives. Carriers of parkin mutations, whether or not they have PD, do not perform differently on neuropsychological measures as compared to noncarriers. The cognitive functioning of parkin carriers over time warrants further study. (JINS, 2011, 17, 1–10)






